Interoperability in Healthcare IT: Medical System Integration and Compatibility Guide

| In this article, we’ll discuss… ✅ Interoperability of health information systems: The purpose and definitions of interoperable medical IT solutions. ✅ Why data interoperability is important in healthcare: Benefits, issues, and challenges for healthcare providers and their patients. ✅ How to achieve interoperability in healthcare: Technologies and models specific to compliance with health IT interoperability. If you want to set up or enhance interoperability between your healthcare systems/products or get any other associated IT services, please contact our experts for individualized consultation! |
What is healthcare interoperability in medical IT systems?
Modern medical computer-aided services exist to support a holistic healthcare strategy. This means that health IT (HIT) integrity must ensure better patient safety, which is the primal goal of digital transformation in healthcare — all software and technology components must organically fit and work together as a whole. Thanks to this formula, the concept of data interoperability in healthcare has emerged.
A single healthcare organization can employ a dozen different medical data-management systems. Usually, this mix of technology is formed over many years of continuous healthcare practice with IT systems, applications, and devices being modified in a variety of ways, like…
- Newly adopted systems and improvements in IT environments
- Upgraded legacy apps and migration to up-to-date platforms
- Software packages updated to later versions
- More sophisticated tools connected and synced with each other
- Outdated medical IT solutions discarded or replaced.
It’s obvious that without healthcare interoperability standards, multiple IT systems created at different times by different vendors would not be able to cooperate.
This would result in an increased number of system errors, lengthy compatibility configuration, and/or the complete inability of certain IT components to interact and exchange medical data. This reality encouraged government-backed regulations for interoperability in healthcare: ?
| The Health Information Technology for Economic and Clinical Health (HITECH) Act of 2009 is considered one of the earliest provisions for developing interoperability standards in digital healthcare technology. This act, coupled with HIPAA requirements for software, has fueled digital transformation and promoted standardization in healthcare systems via full-scale adoption of electronic health records (EHRs) in American hospitals and other medical facilities. EHR or EMR systems owned by different hospitals and medical centers are designed to exchange patient data smoothly. Data formats and processes must be aligned with common rules, including ways to cipher, transmit, and protect healthcare data communications. These healthcare interoperability solutions have consistently led to development and acceptance of system interoperability standards in healthcare, including FHIR and USCDI. |

Before we explain current clinical IT interoperability standards, let’s learn about the key requirements for interoperability in healthcare. There exist several crucial principles specific to medical records that must be respected and managed in the context of all data interoperability solutions in healthcare, including EHRs, computer-aided medical data mining tools, and more:
- Data protection: Healthcare data is always a sensitive matter that requires sufficient levels of privacy and security, according to HIPAA.
- Regulated access: Inability to access healthcare data can potentially cause significant harm to healthcare and patient treatment processes, so data must be not only well-protected, but also readily available to authorized agents.
- Common terminology: Incompatibility and inconsistency in the database fields and concepts used across healthcare organizations and hospital management systems can result in the inability to share, merge, or synchronize health records in data silos.
Objectives for healthcare technology interoperability include:
- Removing barriers and restrictions for different healthcare applications and solutions to interconnect, communicate, and share medical data.
- Making sure that electronic systems from various vendors remain seamlessly compatible despite software updates, code improvements, and system design differences or upgrades.
- Enabling hospitals, private physicians, medical centers, insurance agencies, and medical research institutions to keep their records synchronized and continuously exchange data as required by business protocols.
- Helping patients avoid manual transfer of their records from one healthcare provider to another.
What are the current standards for interoperability in healthcare technology in the United States?
Smooth data exchange between medical systems relies on the following two nationwide interoperability standards in healthcare. Let’s learn more about each of these healthcare interoperability basics.
FHIR (HL7): the medical data shareability framework explained…
HL7 FHIR (Fast Healthcare Interoperability Resources from HL7 International): This open-source tech standard specifies the methodology of healthcare data exchange between different IT systems and concerned parties so they can smoothly interoperate and communicate regardless of how information is stored in different healthcare systems. FHIR [pronounced “fire”] has the following features…
- Ensures standardized medical data structure on the level of technology.
- Employs HTTP-based RESTful application programming interfaces (APIs.)
- Allows secure transfer of clinical and administrative data between authorized users and agents.
- Supports the following electronic document formats: XML, JSON, and RDF (Resource Description Framework.)

USCDI: government-backed health data format explained…
USCDI (U.S. Core Data for Interoperability): A standardized set of patient-centered health data classes. VERSION 3 is the latest edition (2022/23) to be offered as a replacement for the previously adopted Common Clinical Data Set (CCDS.) This list of classes introduces and maintains common terminology to help all healthcare process stakeholders organize and structure healthcare data in their databases in a universally acknowledged manner.
USCDI offers a table of specific classes (each class has its own specifications, like SNOMED International for controlled substances and other matters) with data elements and patient profile options that every healthcare IT system must support, such as…
- Patient demographics
- Allergies and intolerances
- Health status/assessments
- Clinical notes
- Clinical tests
- Diagnostic imaging
- Medications
- Vital signs
- Immunizations
- …and many more.
Before we move on and learn more about interoperability in healthcare information systems, please read a few words about us:
| TATEEDA GLOBAL is a San Diego-based healthcare interoperability service company that offers everything required to develop custom HIPAA-compliant software solutions featuring medical data interoperability and other important functionalities for healthcare businesses and startups. We have skilled healthcare software engineers who can help you with… ✔️ EHR & EMR software development ✔️ DevOps development services ✔️ Custom IoT solution development ✔️ Telemedicine solution development ✔️ Biotech software development ✔️ React.js frontend development Book a free call with our engineer for individualized assistance: ? |

Do You Need a Healthcare Interoperability Solution?
With over 13 years of experience in the biotech and health tech sectors, we are ready to enhance your project with our expert software architects, developers, and QA specialists.
Table of Contents
Levels of Interoperability in Healthcare IT Systems and Applications
Let’s take a look at several healthcare-related parties that benefit from interoperability in healthcare information systems:
- Physicians and ERs
- Hospitals
- Medical centers
- Registries
- Health-tech startups
- Health plans
- Online pharmacy platforms
- Laboratories (Learn more: LIMS development complete guide)
- Employers
- Medical (mHealth) application providers
- Medical research contractors.
In order to explain and support the concept of health IT system interoperability, The American Healthcare Information and Management Systems Society (HIMSS) identified the four main levels of the interoperability model:
#1. Foundational Level: Connectivity Requirements
This is the basic layer of data exchange between separate health information systems. It acknowledges the fact that…
- Different healthcare systems and software must be empowered to exchange USCDI data with all related provisions executed at the earliest stages of their design and mobile application architecture across local networks and Web-based environments.
- The recipient system should be enabled to intake medical data from another system without additional technological tools or manual intervention from users or developers.
- It allows for interconnectivity requirements that let every authorized agent send and accept health data in a fast and totally secure manner, which also requires secure software development practices.
#2. Structural Level: Technical Rules of Data Exchange
This level establishes technical interoperability between healthcare IT systems. It involves…
- Message formats and other technical provisions necessary for smooth data exchange in inner networks and across the Web; FHIR and other HL7 standards to help identify actionable steps to achieve interoperability in healthcare IT operations. Learn more: ➡️ HL7 Integration: How to Build Interoperability Interface for Your Healthcare Systems
- Specific tech definitions of the ways the recipient system(s) read and interpret medical data accurately, including syntax of data fields, informational structures, and anthologies of patient records.
- Every tech aspect that is required to keep precise and correct clinical meaning and the value of every data piece transferred between HIPAA-regulated software.
| TATEEDA GLOBAL has vast experience working with different technical formats, including analog-to-digital signal conversion methods, embedded programming, and biotech hardware projects. For example, we set up interoperability between machine-processing workflows driven by hardware laboratory equipment, human-operated interfaces, and server applications. Learn more: ➡️ Laboratory Test Machine Software Development [Case Study] |
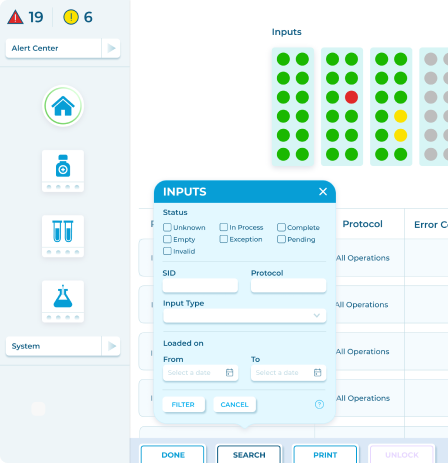

#3. Semantic Level: Human-focused Rules of Data Exchange
When escalated to this level, data-related matters and definitions should agree upon the terms of human cognition, especially medical data visual representation in EHRs and other clinical data management systems. This includes…
- Standardized formal definitions acknowledged by all authorized parties
- Coding vocabularies and dataset codifications in healthcare
- Shared understanding of medical data between all potential users.
#4. Organizational Level: Legislative Preparations
This level covers all legal, social, and organizational provisions and considerations required to facilitate secure data exchange between healthcare actors and medical organizations.
There exist a variety of interoperable software solutions for specific medical domains for example, mental health management apps and they can all fall under specific local and national regulations. This level involves consulting with legal practitioners and negotiations with managerial representatives of all interested organizations.
| Are you interested in the implementation of interoperability in healthcare information systems? TATEEDA GLOBAL has deep expertise and skills in the building of custom HIPAA-compliant healthcare interoperability solutions, including HL7 FHIR-based applications and other health-tech standards. If you need more in-depth consulting for the development of your interoperable healthcare software project, please book a free chat with one of our health-tech experts: ? |

Slava Khristich
Healthtech CTO
Based in San Diego, Slava knows how to design an efficient software solution for healthcare, including IoT, Cloud, and embedded systems.
Why Interoperability in Healthcare IT Is Advantageous: the 3 Major Goals
Why implement and improve interoperability in healthcare organizations? HIT interoperability is necessary for many business purposes: better patient services, reduced healthcare costs, and more. Let’s learn about the benefits of adopting interoperability in healthcare systems…
#1. Better care coordination between healthcare entities
Undoubtedly, it’s convenient when a patient or healthcare organization does not have to transfer their medical records or update each patient record manually across different healthcare parties and their documents. This is an enormous amount of manual work that can be efficiently automated with the help of…
- Real-time electronic synchronization between healthcare records and IT systems, facilitated through the latest telemedicine technologies and healthcare interoperability.
- Custom-tuned collaboration schemes between selected healthcare process actors, government institutions, and other beneficiaries that provide their interoperable software systems.
- EHR/EMR workstations (client applications) interconnected with lab databases, insurance company applications, health plans, patient CMS, and more so all authorized operators can see data updates in all required documents simultaneously.
#2. Higher performance and better treatment outcomes
Technological interoperability in healthcare allows…
- Different physicians and clinical staff to access the latest versions of medical records and see up-to-date information on patient condition.
- Reduction of risks in connection with medical error; elimination of unnecessary testing (e.g., repeated testing for certain types of allergies.)
- Emergency responders to see every important health detail before administering urgent injections and making crucial decisions.
- Reduction of overall time required for working with electronic patient forms and records, thanks to auto-filled documents and forms that extract data from shared databases.
- Nurses and administrators to save time and effort on routine tasks. Specific virtual nursing applications can be integrated with other clinical software, including AI-connected decision systems.
#3. HIPAA compliance and patient data security for all
With its security technologies and provisions, health IT system interoperability allows the following:
- Compatibility of security standards across different healthcare application providers, making sure there are NO weak links between system components that could cause data leaks or other issues.
- Different vendors can develop mutually compatible applications, including medical software and devices that share the same standards and can exchange data without barriers or additional tweaks.
- Physicians and patients can use different applications with the same authorization credentials and protocols to access and manage their records.

Learn more: ➡️ Cloud Computing in Healthcare: 3 Use Cases, Benefits, Features & Best Practices
Challenges of Interoperability in IT Healthcare
Before we consider how to build interoperable healthcare systems, let’s learn more about the main challenges to overcome.
Limited budgets
Everyone suffers from budget limitations, and developing interoperable healthcare systems is not a cheap deal. There are many nuances to be considered:
- Is it a legacy medical system that requires an upgrade in order to be interoperable with modern systems? Do ready solutions like software patches exist for the issue?
- Does it involve the adoption of a new, readymade health information management system? Is healthcare data reformatting and migration from the previous platform required?
- Does the project require the development of a custom medical data system with specific engineering conditions and more?
Solution: Most of these technical nuances must be discussed with a skilled CTO or vendor so the optimal solution that suits your current budget can be found. In most cases, a cost-efficient service can be offered based on your specifics. If you want to discuss your project in the context of matching your budget capabilities, our tech expert is ready to provide you with free health-tech interoperability consulting. Learn more about our regular services: ?
Custom Healthcare Solutions
See how we can engineer healthcare software, validate your ideas, and manage project costs for you.

Medical data being blocked by certain parties
Unfortunately, serious obstacles sometimes arise on the fourth level of the interoperability model: organizational. Certain parties can be reluctant to cooperate and share their databases, connect their data silos to a shared system, and/or disclose sensitive information. In reality, building efficient collaboration between several healthcare business entities is a big project in itself.
There exist specific government-backed protocols for data sharing, but if you want to go beyond them, it’s necessary to work with legal advisors, business leaders, and department representatives to design long-term schemas for safe and mutually beneficial cooperation on medical data.
Solution:
- Identify the benefits of interoperability in healthcare and what each of the participants can win if they share their data in a reasonable way.
- Make sure to work with objections, concerns, and fears (some business concerns may be quite irrational, caused by lack of technical reliance and technological knowledge.)
- Come up with a very specific plan for which data is going to be synchronized, shared, and updated…and how.
- Take into account that some healthcare interoperability service vendors can charge fees for sharing their data and releasing the content of their data silos.
- Consult with skilled engineers to draw up a plan for building a custom healthcare data-sharing solution that follows all HIPAA and interoperability requirements. If you need free tech consulting, please contact us today!
Learn more: ➡️ How to Implement ERP Software Systems for Healthcare
Variability of standards and health information systems
Sometimes, an IT environment in a medical organization can resemble a zoo, with disparate technologies, unique solutions, various modules, and systems added and combined at different times by different specialists…in addition to obsolete or legacy healthcare information-management software. All of this leads to serious difficulties with the implementation of interoperability and measuring its success.
Solution:
- If you don’t have a competent in-house IT specialist/department, hire a professional medical technology outsourcing partner who can audit all involved technologies and come up with a list of interoperability problems.
- Design a plan of what must be done to resolve existing technical problems, including covering formatting gaps between systems.
- Identify the objectives for your healthcare interoperability improvement project, such as reducing manual work, removing security flaws, adding more automation in data-related processes, and so on.
How to Achieve Interoperability in Healthcare IT in 5 Steps
When medical IT systems are not fully interoperable, they can suffer from sporadic or systematic errors, not to mention constant problems with productivity, privacy, and security. All of these risks must be addressed in order to achieve smooth interoperability practices between healthcare applications and digital instruments.
#1. Understand interoperability conceptions
Learn about available standards of medical interoperability and define how well the data stored in your data silos matches the USCDI requirements. Decide whether or not it should be reformatted or reorganized to fit. Other provisions can include…
- Encouraging all collaborating parties and organizations to have a shared understanding and vision of interoperability standards and technologies.
- Educating staff about the concept of using an interoperable system and achieving tech compatibility with health data.
#2. Review and prepare your healthcare data according to industry standards
It is necessary to…
- Audit all digital systems and medical data formats used in your organization.
- Make sure you have a clear plan of what’s lacking on the path to reaching better interoperability between computer-aided healthcare systems and achieving smooth, secure data exchange.
- Make sure to automate data-conversion processes to transform and prepare your records according to USCDI standards.
- Migrate data-management applications to cloud architecture. If you need help with this, please contact us!
| ? Qualified health-tech engineers can investigate this for you and come up with a professional conclusion on which inter-system gaps still exist and must be covered. You can get help from TATEEDA GLOBAL or learn how to find and hire healthcare software developers for your interoperability projects. |

Learn more: ➡️ Healthcare Payroll Software Development
#3. Identify the data to be exchanged
Before building practical interoperability between IT systems in one or several medical departments or organizations, it’s necessary to specify what exact data must be exchanged and agree upon methods, details, and mechanisms deployed between participants so that all potential technical or organizational obstacles can be removed beforehand.
#4. Plan meaningful use of data
Let skilled health data-management engineers design a specific, technically refined way for your data operations to stay lean, rational, and cost-efficient by sending only the necessary details to the correct recipients. Unnecessary data transfers should be excluded so communication channels and computing capabilities can remain uncluttered.
For example, you wouldn’t want to send an entire patient profile to another system when the operator has altered only one field, and you don’t want to send an e-prescription request to all available pharmacies. Instead, you can use a sophisticated engine to question the database for the closest pharmacy that has the required medication in stock, leaving all others aside.
#5. Deploy your IT team to implement the change
- Assign software-development specialists with sufficient knowledge of DevOps, cloud-based computing, and web services to your interoperability improvement project.
- Use project-management methodology to supervise and guide the process of interoperable system integration and configuration according to plan.
- Ensure the security of data in EHR and other interconnected software packages. Test the system, including the data-transfer process between applications. Eliminate all possible gaps.
- Periodically audit interoperability between healthcare IT systems to make sure it works well. This can be executed under medical software maintenance services. TATEEDA GLOBAL has deep expertise with DevOps and healthcare system development services. Please see our portfolio below: ?
Delivered Healthcare Software Portfolio
The leading American healthcare companies benefit from working with us.
Healthcare Interoperability Project Services: Requirements and Estimated Costs
While it’s obvious that integration and interoperability of health data-management systems can significantly improve the outcomes and efficiency of healthcare operations, industry actors must decide if they want to implement interoperable applications, either with in-house means and resources or by delegating these tasks to a managed service provider.
Of course, not all healthcare organizations and companies have equal levels of IT capability, and many do not have it at all. There are three main factors to be considered:
The cost of health IT interoperability integration
Healthcare technology interoperability doesn’t come cheaply or easily, as the process requires the involvement of skilled specialists.
Depending on the scale of the project and other factors, the costs incurred for the development of reliable IT interoperability between healthcare applications (along with required DevOps infrastructure) can be as expensive as 60,000-100,000 USD per medium-sized project per year. However, this is a ballpark estimate that includes average fees for different DevOps infrastructures, licenses, and other crucial expenses.
IT expertise required for healthcare interoperability services
Interoperability requires expensive engineering efforts, including hiring Azure cloud technology experts and developers with specific skills.
That’s why in-house development of IT infrastructure interoperability is beyond the scope and resources of many healthcare organizations. From an HR point of view, building an IT team can take a lot of time, and more than $100,000 in additional expenses per year.
Some of the specialist titles that can be required for this type of project include:
- VPN/network engineer,
- Cloud development engineer,
- DevOps engineer,
- system integrator,
- …and more.
Of course, creating a remote dedicated IT team requires niche expertise, and it can hardly be done by healthcare professionals alone.
Scalability requirements for interoperable IT systems
Of course, there exist many situations for which you must manage the scale of your healthcare IT infrastructure in order to expand it, or reduce costs by scaling it down in a meaningful way.
It’s better to build your whole interoperability infrastructure in a way that tolerates change and won’t entail costly reengineering. This is why a reasonable mix of cloud technologies (like multi-cloud or hybrid cloud) is required, which is to be achieved with custom AWS development services or other platforms.
Additionally, there is a need for continuous uptime network monitoring and other optimization tasks, which require the constant involvement of IT engineers.
| TATEEDA GLOBAL has diversified expertise in cloud-based interoperability requirements and implementation for healthcare organizations. We are NOT providers of IT infrastructure, but we can definitely help you select strategies for the best interoperability solution provider, implementation of all software-related matters and configurations, and continuous monitoring of your healthcare systems. If you want to discuss your project with our health-tech engineer, feel free to contact us. |

Learn more: ➡️ Medical Staff Management Software Development
Accelerate the Process: How to Use APIs in Health IT Interoperability Implementation
Interoperability goals are faster and cheaper to achieve if an organization’s solutions feature open APIs. With these interfaces, developers can assemble interconnected applications with efficient healthcare data exchange and other communication services. The availability of public APIs is an important feature for modern health IT systems, allowing you to build seamless conglomerates of medical data management applications. The most popular EHR providers offer a variety of API-based solutions.
Here are some examples of using APIs for interoperability in healthcare:
Registration dialogs: API-based solutions can be used with EHR systems to add sophisticated user registration functionalities. For example, medical software developers can build a custom multi-factor user authentication portal for patients and physicians and use API to seamlessly integrate with existing EHR or other software.
Medical appointment-scheduling: With the help of custom medical appointment scheduling software development and API integration, it’s possible to integrate time management for physicians and allocate time slots in medical facilities in a wise manner through mutual integration and synchronization with patient profiles, medical records, procedure calendars, e-prescriptions, billing, reminders, and more.
Financial options: Thanks to APIs, it’s simple to integrate billing and insurance claim functionality, safe payment gateways, mobile billing, and other transaction modules. This helps medical centers and hospitals manage and report their financial interactions with patients, insurers, pharmacies, healthcare providers, and other industry agents. This can include automatic generation of invoices to be sent by doctors to insurers or patients automatically. Learn more: Payment System Integrations In Healthcare: The Ultimate Guide
Uncountable capabilities can also be added with APIs, like…
- Hospital information systems for better stock management
- Pharmaceutical manufacturers for medication information
- Pharma retailer systems for e-prescription management
- Public health data management for data analysis and mining
- IoT application and device integration for a variety of purposes
- Specific APIs for interoperability platform integrations, like Azure API for FHIR, IBM FHIR Server, Oracle Healthcare Data Repository, and others.
Examples of Interoperability in Healthcare
Interoperable information systems can be used in healthcare practices in myriad ways. Let’s consider some examples of interoperability in healthcare:
? Building platforms and marketplaces for healthcare services and companies. Different companies can automatically provide up-to-date scheduling information and allow appointment-scheduling from a shared aggregator of offerings.
? Implementing mobile pharma applications for patients that allows them to search for pharmaceutical products in nearby drugstores. This requires pharmacies to share their information on medication in stock.
? Multi-level auto-updating of medical information: A change submitted in one system can entail an update in other interconnected systems. For example, when a physician updates a patient’s diagnosis and issues an e-prescription, a set of sequential actions can be auto-executed to save lots of time…
- an insurance claim can be automatically filed and sent to the patient’s insurer
- e-prescription can be sent to an automatically-selected pharmacy
- all necessary papers for sick leave can be auto-filed and sent to the patient’s employer…and so on.
? Patient data is easily manageable through protected patient portals available on mobile devices and the web in accordance to HIPAA requirements. If you require a secure gateway for patients to access healthcare information, review schedules, and make payments for medical services, our custom patient portal development services are an excellent choice. ?
? Hospitals can send notifications about patient admission, discharge, and transfer to other stakeholders within their healthcare networks.
? Integration with supply-chain platforms for proactive and meaningful coordination between supply-chain partners for delivery and restocking of equipment and medication inventory in hospitals and other medical facilities.
? Integration with government-managed programs, like…
- Medicare Advantage
- Medicaid
- Children’s Health Insurance Program FFS
- Medicaid and CHIP managed care…and more.
How TATEEDA GLOBAL Can Help with Interoperability in Healthcare
Our company has great technical expertise in implementing FHIR-based and HIPAA-compliant interoperable systems. We have built many IT solutions for biotech labs, pharma companies, remote health-monitoring startups, a medical staffing platform, and more.
Services we provide include:
- Custom development of interoperable healthcare data-management solutions
- Implementation of interoperability standards in new and existing products
- Setting up client-server relations between medical software components
- Optimization of data streams and exchange between healthcare applications
- DevOps development in compliance with medical interoperability principles
- Development of IoT and Cloud-based interoperable networks in healthcare
- Medical IT interoperability consulting, testing, and long-term maintenance.
Contact us today for free healthcare software consulting!
FAQ: Interoperability of Health Information Systems
Why is interoperability in healthcare so difficult?
It’s as difficult as any other professional engineering task. In order to make your medical systems efficiently interoperable, you need the help of skilled specialists who can identify current gaps in your IT infrastructure and carry out a specific plan to improve it. You will most likely seek the assistance of experienced DevOps engineers, network specialists, and/or medical application developers.
How does interoperability help in organizational growth?
Frankly speaking, business growth in modern healthcare isn’t really possible without the implementation of medical interoperability methods. All modern practices rely on the application of IT systems, and those who want to develop, facilitate, and expand their healthcare operations need to comply.
How to achieve interoperability in healthcare risk management
The major risks in healthcare are data leaks and misinterpretation of medical data. All these risks can be prevented or minimized with the help of setting up well-tuned interoperability between systems so no valuable data can get lost, misunderstood, or spoiled through incorrect or unreliable communications.
How to achieve interoperability in healthcare quality improvement
You will definitely want to learn more about your patients and business operations by mining data in your custom patient CRM and deriving valuable insights from your database or shared healthcare platforms. With the help of the interoperability feature, you can easily combine different modules, including Big Data analysis services and your healthcare database. If you need consulting on this matter, please contact us!