Bringing AI into Legacy Healthcare Systems: Practical Integration, Risks, and Real-World Gains

This article shows why integrating AI into legacy healthcare systems is a timely move for U.S. providers, what “good” looks like, and how to choose build vs. buy with a pilot-first plan. You will also get a pragmatic scorecard, concrete architecture patterns, and a 30–60–90 pilot blueprint to reduce risk and prove value early.
By the end of the article, you’ll learn the answer in a U.S. context: Where to get integration solutions for legacy healthcare systems? We’re here for you…
U.S. healthcare faces compounding pressure: health spending reached $4.9T in 2023 (17.6% of GDP) and grew 7.5% year over year, while CMS is pushing electronic data exchange and prior-auth transparency through the Interoperability and Prior Authorization Final Rule (January 17, 2024). For CTOs, this makes a strong case for AI integration for legacy hospital IT that adds capacity without ripping out the core.
Many environments remain “legacy” by design: tightly coupled modules and siloed data. Interoperability is improving but unfinished—about two in three hospitals used a FHIR API for patient app access in 2022, and roughly 70% reported engaging in all four domains of exchange in 2023. The gap is the last mile, where integrating AI into legacy healthcare software can automate decisions and close workflow loops using HL7, FHIR, and SMART patterns.
Signals are equally strong on adoption: clinicians and hospitals are already moving. Sixty-six percent of physicians used AI in 2024, and 65% of U.S. hospitals report AI or predictive models integrated with their EHRs. For leaders, the question is sequencing: use a phased AI modernization roadmap for healthcare to decide what to buy for speed and where custom earns its keep for safety, depth, and long-term control.

Do you need AI integration for legacy healthcare systems?
Since 2013, our engineers have delivered custom software solutions for U.S. customers, including system integrations. Let us help you.
Why TATEEDA Is Qualified to Talk About Integrating AI Into Legacy Healthcare Systems
Since 2013, TATEEDA has operated as a custom software development company in San Diego, backed by over 100 senior engineers across Latin America and Europe. We deliver custom healthcare software development services that span EHR/EMR integrations (HL7, FHIR, SMART on FHIR), payer and RCM connections, pharmacy, telemedicine, and mobile. This foundation provides the groundwork required for integrating AI into legacy healthcare systems with HIPAA-ready identity, audit, and change control.
Why our approach fits AI integration for legacy hospital IT:
- Integration-first: HL7 v2, FHIR APIs, interface engines, and SMART apps that sit beside your core.
- Safety built in: least-privilege accounts, PHI redaction, prompt-injection defenses, and human review for clinical actions.
- Proven rollout: 30–60–90 pilots, KPI dashboards, and go-or-grow decisions; plus options to integrate an AI assistant into your healthcare mobile app or integrate AI in custom telemedicine software solutions.
For AYA Healthcare (one of the largest nurse staffing agencies in the U.S.), we delivered AI components for a mature platform: NLP resume parsing, credential OCR with renewal alerts, shift matching, demand forecasting, timekeeping anomaly flags, and a recruiter assistant. The same patterns map directly to integrating AI into legacy healthcare systems inside provider settings, from eligibility checks and prior-auth packets to pharmacy eRx and clinician-ready documentation.
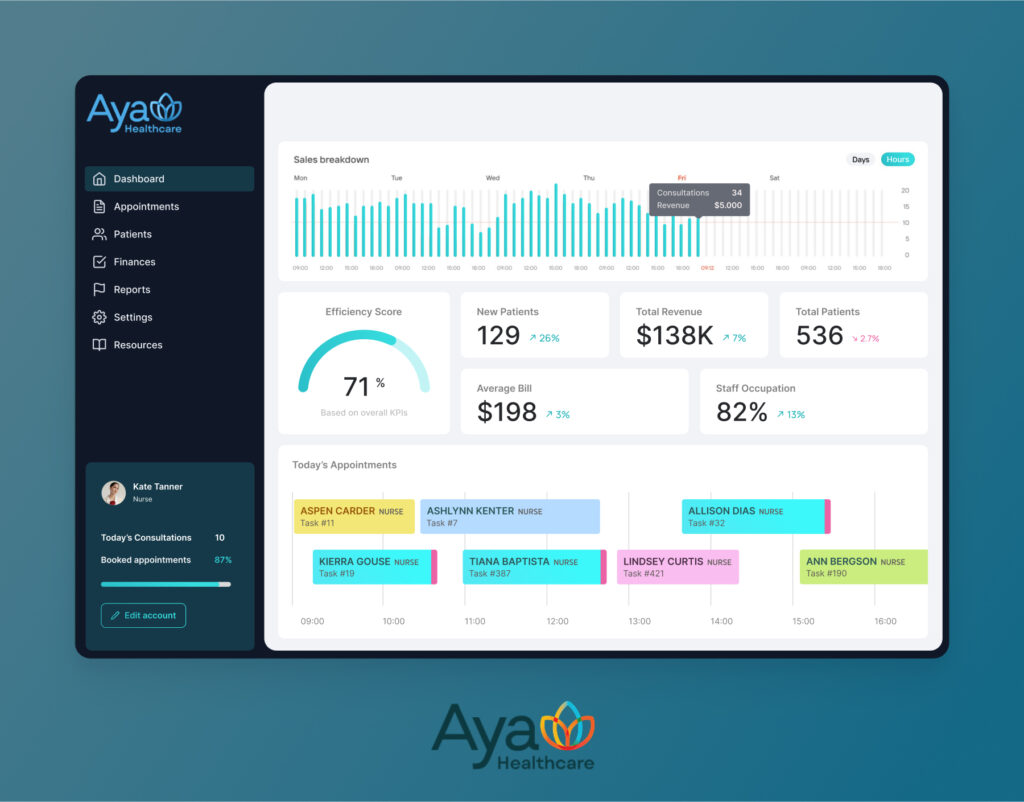
Table of Contents
Why Modernize Legacy Healthcare Software with AI Now: Pressure, Payoffs, and Timing
If you walk into the average hospital IT shop in the United States, you will still find systems whose first commits trace back to around 2010. Many were custom-built for a single organization’s workflows… great for specificity, less great for longevity.
Over time, updates slowed, teams moved on, and maintenance became reactive instead of planned. Under the hood, plenty of codebases still run older stacks such as .NET Framework 4.x, Java 7 or Java EE on WebLogic or JBoss, AngularJS 1.x or Backbone.js, PHP 5.x, and even Python 2.7. The good news is you do not have to rebuild from scratch.
You can layer AI by adding the right APIs, sidecar services, and guardrails to open a path to efficiency across EHRs, custom medical billing systems, and patient-facing apps.
That is why integrating AI into legacy healthcare systems has shifted from optional to urgent. The goal is stability plus lift: augment what already works with automation that reduces clicks, accelerates decisions, and gives patients faster answers.
Think “build around, not through.” Keep your EHR and revenue engines in place, then add safe AI services that call FHIR and HL7 interoperability endpoints, respect HIPAA, and write clean results back into the record. In short, AI integration for legacy hospital IT can expand capacity without risking the core, while your custom patient portal development services surface these gains in a modern, accessible front door.
Quick benefits you can target first:
- Faster documentation via ambient notes and structured summaries ready for review
- Cleaner claims with front-end data checks and prior-auth packet assembly tied to custom healthcare insurance processing software systems
- Earlier risk alerts in monitoring programs with smarter thresholds and clearer escalation
- Shorter wait times through smarter scheduling, reminders, and self-service flows
- Better patient messages that explain benefits and next steps in plain language via custom patient portal development services.
Modernization is also a business decision. For some needs, a platform bot gets you live quickly; for others, safety, audit depth, and multi-system reconciliation argue for custom components. A build vs buy for healthcare AI chatbots discussion lands best with a small pilot that measures time to resolution, containment, denial reduction, and safe-action rates. Scope tightly, decide in weeks, then scale what wins as part of a phased AI modernization roadmap for healthcare.
| Option | Speed | Control | Typical fit |
| Preconfigured bot | Fastest | Low | FAQs, basic scheduling, simple Q&A |
| Configurable platform | Medium | Moderate | Pilots, phased rollouts, moderate integrations |
| Custom build | Slower start | High | Deep EHR ties, prior-auth logic, strict governance |
When timelines are tight and integrations are shallow, buy a starter. When safety rules, multi-system reconciliation, and audit depth matter, build the parts you must control.
Slava K., CEO, TATEEDA
Timing matters because every month of delay keeps manual work in place. Start where the impact is obvious, then modernize legacy EHRs and EMRs with AI for more complex workflows, such as prior authorization or documentation at scale.
As you expand, favor legacy system AI integration with FHIR and HL7, and do not forget the patient front door. You can also integrate an AI assistant into your document workflows and your portal to extend the same gains to refills, reminders, payments, and virtual visits.
Readiness Check for Legacy Healthcare Software with AI: Code, Data, and Compliance Posture
Before you add intelligence, make sure the foundation will hold. A quick but thorough assessment prevents “AI on sand.” For AI integration for legacy hospital IT, look first at code stability and the interfaces that feed and accept clinical data. Old does not mean unsafe, yet unsupported runtimes, brittle batch jobs, and hand-rolled parsers often do. Confirm you can read and write through stable endpoints, and that timeouts, retries, and logging exist where traffic is heavy. Teams working on custom hospital information software development often find these checks surface integration hotspots early, so fixes can be prioritized.
Data decides what your assistant can safely do. Map lineage from source to store, then verify the ETL paths into your warehouse. For legacy system AI integration with FHIR and HL7, check actual coverage. Do you have FHIR read and write for the resources your use case needs, or only read access? Are HL7 v2 feeds complete for ADT, orders, and results? For outpatient workflows, AI can be used to enhance ambulatory management systems by enriching schedules, eligibility checks, and visit documentation with EHR-safe context. Compliance wraps it all. HIPAA rules, a signed BAA, encryption in transit with TLS 1.2 or higher, encryption at rest, and a real audit trail that captures who did what and when.
Technical checks you can complete in a week:
- Code and services: Produce a runtime inventory with versions for the app server, language, and frameworks. Flag end-of-life items and create a patch plan. Run a smoke test and a short baseline load test to capture error rates, p95 latency, and resource spikes. Note container readiness and any hardcoded file paths or local state that would block scaling.
- Interfaces: List the exact FHIR resources and verbs available, such as Patient, Coverage, Appointment, and Claim, with read and write where needed. Capture HL7 v2 message types like ADT^A01 admit, ADT^A03 discharge, ORM orders, and ORU results with their throughput and error handling. Record API rate limits, sandbox tenant details, and health endpoints for monitoring.
- Data: Draw a lineage diagram from source systems into the warehouse. Document ETL schedules, failure alerts, and data quality checks. Define de-identification for model evaluation using a Safe Harbor approach. Verify PHI masking for logs and analytics tables, and specify retention and purge rules.
- Security: Confirm role-based access controls for every integration. Use least-privilege service accounts with scoped permissions. Store secrets in a vault with rotation enabled. Enforce TLS in transit and encryption at rest. Prove audit log integrity by exporting to write-once storage and testing an access review.
- Environments: Load a representative synthetic dataset that includes edge cases like null insurance, duplicate MRNs, and long medication lists. Gate risky actions behind feature flags. Define a rollback playbook that covers application binaries and database migrations. Turn on tracing so every request carries a correlation ID end-to-end.
| Asset | “Good enough to start” bar |
| EHR connectivity | FHIR reads plus at least one safe write path in a sandbox tenant |
| HL7 v2 feeds | Stable ADT plus one additional stream needed by the use case |
| Data warehouse | Ingested clinical and billing data with PHI masking for analytics |
| Security | BAA in place, TLS, at-rest encryption, RBAC, central secret storage |
| Observability | Request tracing, error dashboards, alerting, and audit exports |
Ship the pilot only when you can prove where the data came from, who touched it, and how it moved. That is how integrating AI into legacy healthcare systems stays safe from day one.
Slava K., CEO, TATEEDA
If you meet this bar, you are ready for API-first AI integration for legacy healthcare stacks. Stand up a non-production assistant with synthetic data, then graduate to a limited live cohort once logs and KPIs look clean.

Architecture Patterns for Upgrading Legacy Healthcare Software with AI: Build Around, Not Through
The safest way to add AI is to leave the core where it is and attach new capabilities at the edges. Decouple legacy core and add AI sidecar services that call approved endpoints, apply policy, and return structured results. The EHR, billing system, and portal continue to run. The sidecars handle recognition, reasoning, and tool use, then write back through FHIR or queue HL7 updates through your interface engine.
Use proven integration primitives. SMART on FHIR launches let you place assistant features right inside the clinician’s workflow. HL7 v2 feeds move admissions and result events into your AI services for context. An API gateway fronts the assistant with OAuth 2.0 or OIDC so identities and scopes travel correctly. Add retries with backoff, enforce idempotency with request keys, and log every action with a correlation ID so you can trace a decision end-to-end. This same pattern extends to patient engagement software solutions by enabling secure messaging, refill prompts, and appointment follow-ups that stay in sync with the source of truth.
Standard components for a stable AI retrofit
- Tool router: a small service that validates input against a strict schema, chooses the next tool, and enforces timeouts and circuit breakers. It should record every call with request and response hashes, block prohibited actions by role, and fall back to a human task when a policy check fails.
- RAG service: retrieval augmented generation that only pulls from a vetted knowledge index such as clinical policies, formularies, and internal guides. Use chunking with embeddings, attach citations to every answer, and version the corpus so you can reproduce past results during audits.
- Vector store: pgvector inside Postgres or a managed store like Pinecone to embed policies and reference documents. Strip PHI before indexing, define refresh cadences, and keep an index of document provenance so you can retire stale content cleanly.
- Queue and cache: a durable queue like SQS or RabbitMQ to coordinate multi-step work, plus an in-memory cache such as Redis to cut latency for stable lookups. Add backpressure handling and dead-letter queues, and make cache entries short-lived to avoid serving outdated eligibility or formulary data.
- Observability and safety: OpenTelemetry tracing, metrics, and structured logs for every prompt, tool call, and write-back. Add prompt and output filters, a small set of adversarial test cases, drift monitors on embeddings and answers, and a kill switch that immediately disables risky actions while leaving read-only features available.
| Pattern | Where it helps | Notes |
| AI sidecar microservice | EHR documentation and messaging | Keeps core untouched while adding summaries and drafts |
| Event stream from HL7 v2 | RPM alerts and triage | Feed ADT, orders, and results into the assistant for context |
| SMART on FHIR app | Clinician inbox and chart | Launches inside the EHR with secure context and scopes |
| Idempotent write-backs | Claims edits and prior auth | Prevents duplicates if retries occur during outages |
Build around the core so the hospital can keep seeing patients while you improve the plumbing. In plain terms, that means build around, not through, legacy systems with AI services.
Slava K., CEO, TATEEDA
With this pattern, you can migrate legacy HL7 and FHIR workflows to AI-enabled services one slice at a time. Start with ambient notes or benefits checks, then extend into prior-auth packets and documentation at scale. The result is an AI retrofit for legacy EHR and EMR platforms that raises capacity without risking the systems that keep the doors open.
Phased Path for Legacy Healthcare Software with AI: Pilot First, Then Scale
Start small, learn fast, then expand with confidence: A pilot-first AI program for legacy healthcare systems lets you test one workflow under real load while controlling risk. Keep your core stable and attach capability at the edges using API-first AI integration for legacy healthcare stacks. The goal is proof, not perfection: run a 30–60–90-day AI pilot for legacy EHR modernization:
| Phase | Primary goals | Key deliverables | Owners |
| Days 0–30 | Stand up MVP for one workflow | Sandbox connectivity, safe-action gates, baseline prompts, KPI plan | Product owner, security lead |
| Days 31–60 | Run controlled live traffic | A/B rules, KPI dashboard, drift and error logs, weekly reviews | Data steward, clinical lead |
| Days 61–90 | Harden and decide | Remediation plan, integration backlog, TCO view, go or grow decision | Steering group |
KPI menu to watch:
- Containment rate: percent of inquiries resolved without human handoff
- Time to resolution: median minutes from first contact to outcome
- Denial reduction: change in payer denials on touched encounters
- Readmission risk capture: percent of flagged patients reviewed within policy windows
- Safe-action rate: percent of actions passing policy checks.
Go or grow rules:
- Go with the platform where KPIs meet targets and integrations stay straightforward
- Grow into custom where safety, prior-auth logic, and deep writes demand control under a phased AI modernization roadmap for healthcare
- Defer where error patterns persist or business value is unclear.
“Measure before you multiply. Ship one clean slice, learn from the logs, then choose speed or control with your eyes open.”
Slava K., CEO, TATEEDA

High-Value Use Cases: How Adding AI to Legacy Systems Changes the Outcomes
Modernization works best when tied to specific wins. These examples show how integrating AI into legacy healthcare systems can deliver visible gains. Figures are directional, based on typical baselines, and will vary by environment.
Clinical:
- Ambient notes and summaries inside a SMART on FHIR app. Physicians review drafts instead of typing from scratch. Documentation time drops 25–40 percent when you integrate AI in legacy EHR systems using safe read and write scopes.
- CDS prompts are grounded in retrieval from policies and pathways. Clinicians see concise suggestions with citations. Interruptions go down, and adherence to local guidance improves.
- Imaging triage and AI-powered medical diagnostics assist. Alerts route urgent studies to the front. Average time to first review decreases by 10–20 minutes once you migrate legacy HL7 and FHIR workflows to AI-enabled services.
Operations:
- Prior authorization assembly. Gather evidence, draft forms, and package for staff approval. Denials on targeted lines fall 10–20 percent after clean packet routing.
- Claims edits and patient billing Q&A are tied to your rules engine. Fewer back-and-forth calls, clearer bills, higher first-pass yield.
- Inventory checks with reorder prompts based on real consumption. Stockouts drop, and on-hand shrinkage eases. For pharmacy operations, custom pharma software development services can integrate dispensing systems, 340B accumulators, supplier feeds, and formulary data to improve forecasting, automate batch purchasing, and flag recalls in real time.
Access and engagement:
- Triage, scheduling, and refills are exposed through the portal and contact center. No-show rates improve 8–15 percent with smarter reminders and standby logic.
- Integrate an AI assistant into your healthcare mobile app and telemedicine flows to mirror the same outcomes on the patient’s phone. Secure messaging answers common questions and hands off safely when policy requires.
For older stacks, an AI retrofit for legacy EHR and EMR platforms or AI modernization for legacy healthcare platforms adds these capabilities without a rebuild. Treat each use case as a slice, then stack the slices as confidence grows.
Guardrails, Costs, and the Extension Playbook for Legacy Codebases
Safety comes first. You can upgrade outdated healthcare software with AI while keeping clinical and financial systems steady if you place guardrails before growth.
Safety and governance checklist:
- Human in the loop for clinical advice and outbound documentation
- Prompt injection defenses and output filters, plus adversarial test cases in CI
- Redaction for PHI in prompts, logs, and analytics tables
- Audit logs that are tamper-evident and exported to write once storage
- Model evaluation for accuracy, drift, and bias, with monthly reviews.
Cost lenses to model:
- Licenses and usage for model access and platform fees
- Integration effort to decouple legacy core and add AI sidecar services that call FHIR or queue HL7 v2
- Data cleanup and ETL fixes to make lineage and retention defensible
- Change management and training so staff adopt new flows
- Ongoing MLOps for corpus refresh, prompt updates, and evaluation runs
All figures are directional. Real totals depend on use case count, payer mix, EHR scope, interface engine coverage, and your internal capacity.
AI extension strategy for legacy codebases
| Strategy | When to prefer | Typical components |
| Platform connectors first | You want speed, and your needs match existing features. Interfaces are light and read-heavy. | SMART on FHIR launch, vendor SDK, policy-backed RAG, audit export, identity via OAuth 2.0 or OIDC |
| Custom AI sidecars | You need deep writes, strict policy checks, or multi-system reconciliation that a platform cannot expose. | Sidecar microservices, API-first AI integration for legacy healthcare stacks, idempotent write-backs, retries, correlation IDs |
| Hybrid staged extension | You need fast wins now and control later. Start on a platform and add custom slices where outcomes depend on fine control. | Platform bot for front-door tasks, targeted sidecars for prior auth and documentation, shared observability and safety services |
Keep the architecture simple. Build around, not through legacy systems with AI services that sit beside your EHR and billing engines. Use a phased AI modernization roadmap for healthcare to decide where platform connectors are enough and where custom sidecars are warranted. That gives you an AI upgrade path for aging healthcare applications without a rebuild and a plan you can defend to clinical leaders and finance.

Final Word: Upgrade Legacy Systems with AI, Safely and Pragmatically
You have the plan. Start with a focused pilot, measure hard KPIs, then expand into the high-value slices: ambient notes, prior-auth assembly, claims clarity, patient access, and mobile or telemedicine touchpoints. Keep the core stable, attach AI sidecars, use SMART on FHIR and HL7 v2 where it fits, and build guardrails first so every action is observable, reversible, and policy-compliant.
TATEEDA can help. Since 2013, our San Diego, California headquarters has led nearshore delivery with senior software engineering teams across LATAM and Europe. We handle integrating AI into legacy healthcare systems as well as AI integration for legacy hospital IT: identity and SSO, HIPAA and BAA, audit trails, safe-action gates, and model evaluation.
If your goal is to upgrade outdated healthcare software with AI or modernize legacy EHR and EMR with AI, we can move from readiness check to a 30–60–90 day proof quickly, then scale what works.
We handle full-stack integrations for US clients. We build and maintain connections to leading platforms and the plumbing that ties them together:
- Vendors and platforms: Optum integration, Waystar integration, Allscripts integration, Oracle Health (Cerner), and athenahealth integrations.
- Standards and engines: HIPAA compliance, FHIR and HL7 endpoints, interface engines, and payer portals.
- Patient front door: patient engagement software solutions for web and mobile.
What this enables in your stack:
- Eligibility and prior authorization with cleaner packets and status tracking
- Claims status and billing with clearer patient Q&A and fewer handoffs
- Scheduling and refills with smart reminders and safe write-backs
- Secure messaging inside your portal or mobile app.
If you’re ready to modernize the right way, we’ll map outcomes, integrations, and safety controls and run a 30–60–90-day pilot to prove value, so contact us to get started.











