How to Integrate Waystar with Custom Healthcare Applications

This article offers a comprehensive technical guide to Waystar integration services for custom healthcare applications, detailing how to embed eligibility verification, claims submission, payment posting, authorization workflows, and EHR/PM system connectors into custom healthcare software solutions while showcasing TATEEDA’s end-to-end expertise.
Waystar stands as one of the largest SaaS-based revenue cycle management (RCM) platforms in the United States, processing claims for over half the country’s population and connecting to more than 5,000 payer endpoints. Trusted by over 1 million providers and 1,000+ hospitals, Waystar’s network spans commercial insurers, Medicare, Medicaid, and regional plans, giving it an unparalleled market share in clearinghouse services.
Through Waystar integration services for custom healthcare applications, organizations embed eligibility checks, claim submission, payment posting, and denial management directly into their existing software ecosystems.

If you require immediate engineering help to integrate Waystar system with a healthcare application of your choice, please contact our health tech development experts.
At its core, Waystar offers a unified API layer, batch file interfaces, and HL7 integrations that can be woven into any custom EHR, practice management system, telehealth platform, or patient portal. For instance, Waystar Epic integration services surface eligibility data and claim statuses right within the Epic workflow, while Waystar eClinicalWorks integration services allow ambulatory practices to submit claims and retrieve remittances without leaving their native interface. Waystar MEDITECH integration services extend these capabilities into community hospitals, and Waystar practice management integration services tie into legacy and niche PM systems.
Healthcare IT teams need Waystar RCM integration solutions because building direct payer connections is time-consuming, error-prone, and costly. By leveraging Waystar’s established network and continuously updated rule engines, developers can accelerate custom software delivery, maintain compliance with X12 and HIPAA standards, and focus on user experience rather than transaction plumbing.
Integrating Waystar authorization integration services ensures prior authorizations flow seamlessly, and Waystar patient payments integration services power embedded patient billing and self-service portals. In short, custom applications become not only clinical tools but full-fledged financial engines when paired with Waystar.
Why Is TATEEDA Qualified to Talk About Custom Waystar Integration?
TATEEDA teamed up with AYA Healthcare—one of the nation’s largest travel nurse staffing firms—to build a resilient, multi-tier RCM ecosystem based on Waystar integration services for custom healthcare applications. Our engineers consumed Waystar’s RESTful and batch APIs to automate claim submissions (X12 837), remittance posting (X12 835), and denial management, while HL7 interfaces kept scheduling and patient data in sync.
We layered in mobile dashboards for on-the-go claim status checks, embedded Waystar patient payments integration services in the nurse portal, and drove real-time KPIs via event-streaming analytics. That end-to-end, scalable delivery of Waystar custom software integration services proves TATEEDA can architect and execute your most complex Waystar integration projects.
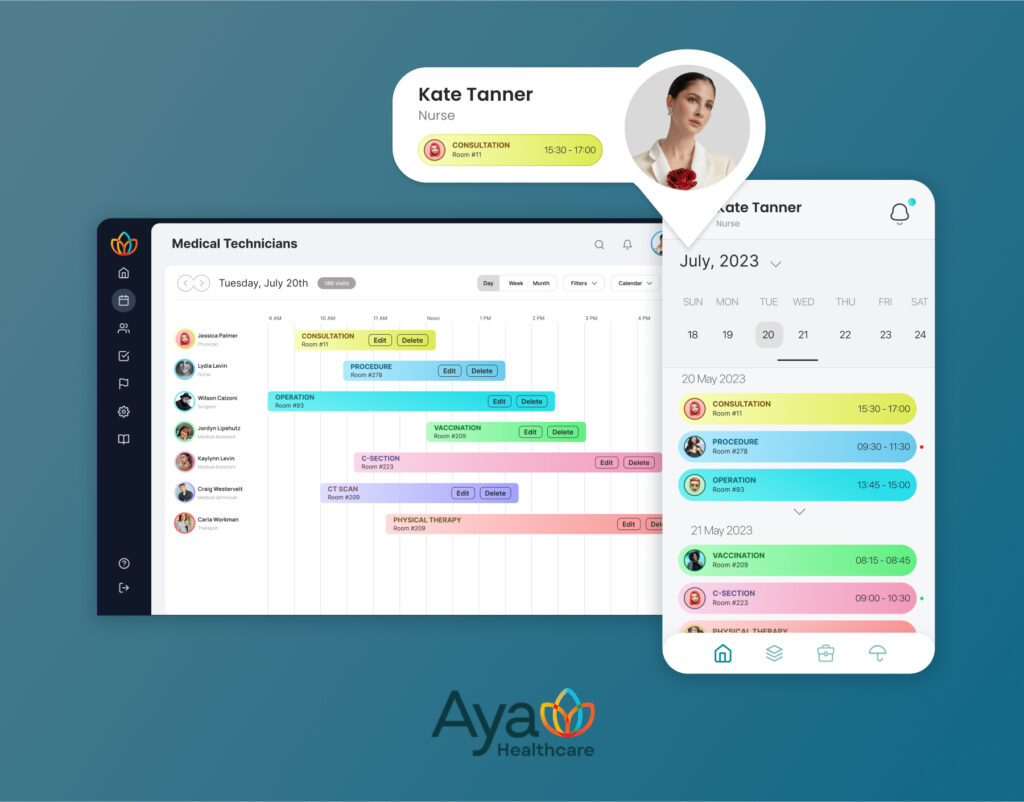
Table of Contents
How Waystar Integration Works for U.S. Healthcare Providers
Waystar exposes a variety of integration methods—RESTful APIs, SOAP web services, SFTP batch exchanges, and HL7 feeds—to connect custom software with critical RCM functions. These Waystar integration services for custom healthcare applications enable real-time and batch data flows:
- Eligibility Verification (270/271): Instant checks using REST endpoints or HL7 ORM messages to confirm coverage before scheduling or registration.
- Claim Submission (837): Real-time API calls or nightly batch uploads (SFTP) of X12 837 files, with immediate feedback on claim acceptance or rejection.
- Claim Monitoring (276/277): Automated status sweeps that poll payer systems for claim adjudication updates, reducing manual follow-up.
- Payment Posting (835): Remittance data retrieval via APIs or file transfers, auto-matching payments and remitting advice to transactions in custom ledgers.
- Denial & Appeal Management: Denial codes and explanation-of-benefit details flow through APIs, enabling workflows to triage and auto-populate appeal forms.
- Prior Authorization (278): Programmatic submission and tracking of authorizations to payer systems, integrated directly into order-entry screens.
- Patient Billing & Payments: Embedded payment portals via Waystar patient payments integration services, allowing online payments, payment-plan setup, and co-pay collections.
These connections can dramatically transform custom healthcare applications in many domains:
- Custom EHRs:
By employing Waystar Epic integration services or Waystar Cerner integration services for revenue cycle management, customized EHR development solutions embed payer checks and claim workflows into the clinical interface. Providers see eligibility alerts when ordering labs, and billing staff launch claims directly from visit notes, improving first-pass acceptance rates. - Practice Management Systems:
Practices using PM software (from solutions integrated with Allscripts to niche vendors) benefit from Waystar practice management integration services that automate daily claim batches, remittance imports, and AR aging reports. Automated scrubbing and real-time status screens cut down follow-up calls and accelerate cash flow. - Ambulatory & Specialty Apps:
Waystar eClinicalWorks integration services and Waystar MEDITECH integration services bring RCM features to ambulatory surgery centers, dental clinics, and rehab practices. These integrations unify scheduling, billing, and patient statements in one UI, so staff manage patient flow and revenue in sync. - Patient Portals & Mobile Apps:
When paired with Waystar patient payments integration services, custom patient portal solutions display balances, upcoming charges, and enable secure online payments. Mobile apps can push payment reminders via SMS, linked to Waystar’s payment APIs for seamless checkout experiences. - Telehealth & Virtual Care Platforms:
Waystar authorization integration services ensure virtual visits are covered. Prior authorization checks prevent claim denials, and payment links embedded in telehealth workflows let patients settle co-pays immediately post-visit. - Analytics & BI Dashboards:
Ingesting 835 remittances and 277 status data via Waystar RCM integration solutions fuels dashboards that track key metrics—clean claim rates, denial trends, AR days. Finance teams and executives gain real-time visibility without manual data exports. - AI Agents & Virtual Assistants:
Using Waystar custom software integration services, you can embed custom AI agent solutions that call Waystar’s REST and batch APIs to automate member support. Agents authenticate via OAuth2, parse queries with an NLP engine (e.g., OpenAI or Azure Cognitive Services), and request Eligibility (270/271), Claim Status (276/277), and Payment data. An event-driven middleware (Kafka or AWS SNS) queues requests, while Redis caches common lookups to reduce API traffic. Responses—delivered via chatbot widgets or SMS—are logged to an ELK stack for audit. This blend of Waystar RCM integration solutions and AI assistants cuts call center volume and gives members 24/7 self-service.

Learn more: ➡️ AI-Smart Custom Ambulatory Software Development
Partner Ecosystem:
These integrations are delivered by a range of partners, including:
- EHR & PM Vendors (Epic, Cerner, eClinicalWorks, Meditech) with built-in connectors;
- Integration Platforms (MuleSoft, Redox) that mediate between Waystar and custom code;
- Custom Software Firms (like TATEEDA) offering end-to-end Waystar custom software integration services;
- Consultancies and SIs specializing in healthcare RCM.
Step-by-Step Guide to Waystar Integration
| Waystar Feature | Description | Integration Use |
|---|---|---|
| Eligibility API (270/271) | RESTful endpoint for real-time eligibility inquiries. | Embed in registration, scheduling, and order forms for instant coverage checks. |
| Claim Submission API (837) | Submit professional and institutional claims via API or SFTP. | Automate daily claim batches from custom billing modules. |
| Claim Status API (276/277) | Poll payers for claim adjudication updates programmatically. | Drive AR workflows by surfacing status in dashboards. |
| Remittance API (835) | Retrieve electronic remittance advice in JSON or X12 format. | Auto-post payments to practice accounting or ERP systems. |
| Attachments API | Upload supporting documents (e.g., prior auth, clinical notes) via API or secure file transfer. | Attach required docs to claims without manual faxing. |
| Prior Authorization API (278) | Request and monitor authorizations through real-time API calls. | Integrate auth checks into telehealth or care-pathway workflows. |
| Patient Payment API | Process patient credit card, ACH, or payment-plan transactions. | Build custom portals and mobile apps for self-service payments. |
| Denial Management Endpoints | Receive denial codes, reasons, and appeal data via API. | Auto-route denials to workflows and prefill appeal forms. |
Learn more: ➡️ Nearshore Software Development Services
Waystar System Implementation Steps:
- Provisioning & Credentials: Sign up for Waystar Partner Portal, obtain API keys, and configure SFTP accounts.
- Sandbox Testing: Use Waystar’s test payers for 837/835, 270/271 scenarios. Validate JSON schemas and X12 translations.
- Authentication: Implement HMAC-SHA256 or OAuth2 (as required) for API calls. Secure credentials in vaults.
- Data Mapping: Create transformation services to convert internal models to Waystar’s JSON/X12 formats.
- Error Handling: Incorporate retry logic for HTTP 429 and transient errors; log all transactions with correlation IDs.
- Performance Tuning: Cache eligibility responses, batch large claim uploads during off-peak windows.
- Monitoring & Alerts: Set up API health checks, SLA dashboards, and PagerDuty alerts for failures.
- Go-Live & Support: Switch to production endpoints, schedule routine audits, and maintain a support hotline with Waystar.
Our Custom Software Development Services with Waystar Integration
Integrating Waystar’s powerful RCM engine into custom healthcare software—from EHRs and practice management systems to patient portals and telehealth apps—eliminates the complexity of direct payer connections while driving efficiency, compliance, and revenue performance.
Through Waystar integration services for custom healthcare applications, organizations gain:
- Faster Eligibility & Claims: Instantly verify patient coverage with real-time 270/271 API calls embedded in registration and scheduling workflows, then automatically batch-submit 837 claim files via SFTP or REST during off-peak hours. This end-to-end automation slashes manual data entry, cuts cycle times, and ensures claims are in the payer queue within minutes of service completion.
- Reduced Denials: Drive clean-claim rates above 98.5% by integrating Waystar’s AI-powered rules engine into your claim prep process. Customizable edit lists and Altitude Assist™ automatically flag missing or mismatched codes, enforce payer-specific business rules, and suggest corrections in real time—eliminating the need for repetitive claim rework and reducing write-off risk.
- Seamless Payments: Embed Waystar patient payments integration services directly into your patient-facing portals and mobile apps. Enable online credit-card or ACH transactions, payment-plan setup, and co-pay collection workflows. Real-time payment posting via 835 APIs or secure file transfers ensures revenue is recorded instantly and reconciled against claim records without manual intervention.
- Complete Oversight: Gain full visibility into every revenue cycle stage with integrated dashboards that combine claim status (276/277), remittance details (835), and denial analytics. Automated alerts notify finance teams of stalled claims or high-risk denials, while appeal management endpoints let staff initiate and track appeals from within your own software.
Why Choose TATEEDA for Waystar Integration Services?
- Solution Architecture & Roadmaps
Our architects and business analysts conduct in-depth discovery workshops to map your existing systems, define data flows, and identify bottlenecks. We produce detailed sequence diagrams, API dependency matrices, and multi-phase implementation plans that align Waystar’s capabilities with your clinical and financial workflows. - Custom API Development & Security
Senior backend engineers build and secure every integration point—implementing OAuth2 token management, HMAC-SHA256 signing, and robust SFTP channels. We deliver reusable SDKs, microservices for JSON-to-X12 conversion, and event-driven architectures that keep your data safe and ensure zero-downtime deployments. - Sandbox Validation & Performance Testing
Our QA and performance teams script comprehensive test suites (Postman, JMeter) to simulate real-world volumes of 270/271, 837, and 835 transactions against Waystar’s sandbox. We verify error-handling logic, measure API latency, and stress-test batch pipelines to guarantee sub-second responses and batch windows that fit your operational SLAs. - HIPAA & X12 Compliance Expertise
Compliance specialists enforce administrative, physical, and technical safeguards across your integration. We ensure all data in transit is encrypted (TLS 1.2+), at rest is secured (AES-256), and that audit logs meet HIPAA, SOC 2, and X12 requirements. Our documentation and validation artifacts support certification and audit readiness. - Ongoing Support & Optimization
After go-live, our DevOps and support engineers monitor API health with Grafana dashboards, manage auto-scaling policies, and resolve incidents via PagerDuty. We periodically review claim and payment performance metrics, tune rule engines as payer policies change, and roll out incremental enhancements under a continuous-improvement framework.
Partner with TATEEDA to deploy Waystar Epic integration services, Waystar eClinicalWorks integration services, Waystar MEDITECH integration services, Waystar authorization integration services, and Waystar custom software integration services, unlocking a unified revenue cycle experience within your bespoke healthcare applications.

Would You Like to Integrate Waystar with Custom Healthcare Applications?
TATEEDA has been helping US healthcare companies since 2013.











