Medical Software Testing and Quality Assurance in Medicine

In this article, we’ll delve into matters of medical software quality assurance. You’ll learn why testing is necessary for every new software system to be implemented in a healthcare organization, how the testing process should be organized to comply with security standards and regulations, and many other details.
Like numerous other fields, the healthcare industry employs technology designed to deliver high-quality services to patients, streamline data transmission, and simplify access to important information. In this case, it also elevates the quality of diagnostics and treatment.
Countless innovative projects, software products, and medical devices have emerged in recent years. Rapid technological advances have made medical devices and software more complex and sophisticated than ever.
Since these changes not only deliver value but also pose risks, a strict regulatory framework is needed to prevent low-quality products from appearing on the market.
Before releasing any item, developers need to perform thorough testing to detect and effectively neutralize any drawbacks, confirm compliance with high market standards, and meet the strict requirements of regulatory bodies. Partnering with a skillful healthcare software development company can ensure that your medical software undergoes rigorous quality assurance processes, leading to a reliable and compliant product.
Frequent changes in the global and national software development landscape and slow-to-adapt regulatory bodies complicate the delivery of finished products to target markets. However, thorough medical software testing and official certification are necessary for products to enter the market legitimately and avoid legal issues in the future.
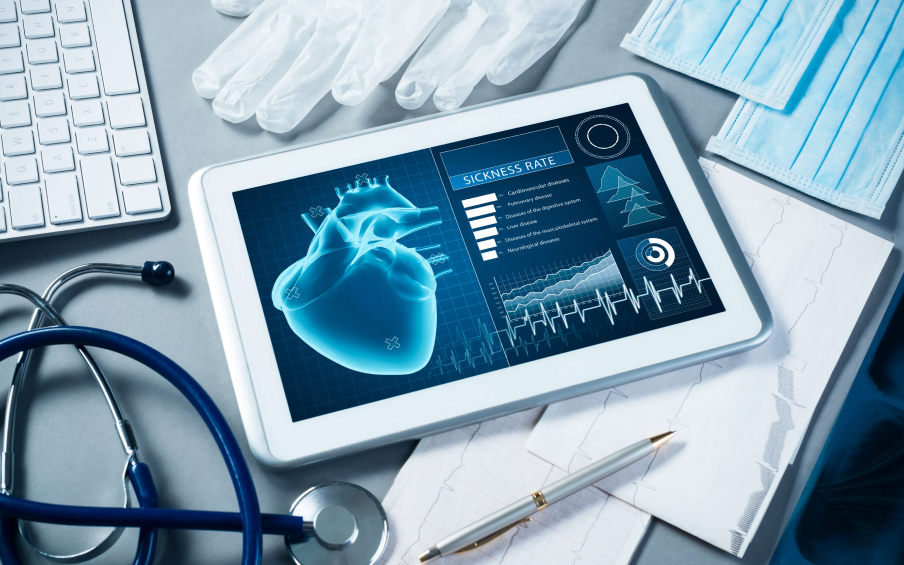
Table of Contents
How the Quality Assurance Process in Healthcare Works
There are official specifications for different types of medical software and devices, developed by regulatory bodies to safeguard high-quality standards in the market for medical products and services. The requirements of regulatory bodies focus primarily upon the accuracy of diagnostics and data transmission, high performance, and safety. The FDA recently designated software as a medical device.
Medical software providers should keep these requirements in mind while they are still in the planning stages, since it can be much more expensive and tedious to remodel existing architecture and features when a product has already reached the later stages of development.
Monitoring a product’s quality throughout the entire software/device development cycle as well as during transportation, warehousing, and implementation is called quality assurance (QA).
A sound QA strategy allows software companies to approach the medical software testing phase fully prepared and equipped with the necessary toolkit. This includes a clear idea of the existing standards and validation criteria their products have to meet. QA reduces development time and costs while allowing innovative companies to focus upon the research and design of new useful solutions rather than fixing errors.

Slava Khristich
Healthtech CTO
Based in San Diego, Slava knows how to design an efficient software solution for healthcare, including IoT, Cloud, and embedded systems.
Types of QA in the Healthcare Industry
- Medical software testing and quality assurance. This refers to the testing of software products created to enhance medical facility workflows and/or individual healthcare, including telehealth applications, mobile health monitoring apps, hospital information management systems (HIS/HIMS), electronic medical records (EMR) management systems, and many others. If you’re looking to augment your current medical software project team with skillful QA engineers, hire TATEEDA. We offer healthcare software project reinforcement services as well as custom software development projects, including QA/testing of medical software, project management, full-cycle development, and UI/UX design.
- Medical device software verification validation and compliance: Another class of software products to be tested includes systems and controllers that maintain the functionality of healthcare devices. These range from high-end hospital diagnostic equipment to personal AI-powered insulin pumps and asthma-monitoring and prevention devices. The process consists of medical device testing plus software testing to make sure both layers (hardware and software) are perfectly synchronized. The regulatory requirement for medical software quality assurance is the IEC 62304 standard, which is recognized internationally. This includes the U.S. and the E.U.
- Medical device testing is quality assurance for medical equipment alone. The standards for medical device software testing and compliance include IEC 60601.
The Value of QA for the Healthcare Industry
Healthcare software quality assurance benefits the healthcare industry in a number of ways:
- Ensures the seamless operation of all medical software solutions, including patient apps, clinical databases, customer relations management systems, and medical equipment software.
- Establishes reliable connections in device networks.
- Helps developers prepare for compliance testing with major regulatory frameworks.
- Eliminates weak links, prevents software failure, and ensures upscale performance.
- Helps predict the behavior of medical software in various real-life scenarios.
Inattention to QA issues can result in a low-quality end product, undetected bugs, incorrect diagnoses, and counterproductive treatments that actually harm patients rather than solving their health problems. Quality assurance practices in healthcare software development are a must, not an option.
The tiniest details must be scrutinized to comply with strict standards while outrunning the competition and delivering the best products to the market. Healthcare software testing prevents costly medical errors and potentially irreversible harm to patients. QA reporting is also used to assure the investors and clinics who purchase your products that your company works in good faith.

Reasons to Invest in Medical Device QA Services and Software
Software quality assurance procedures in healthcare and the generation of supporting documentation take a lot of time and effort, distracting device manufacturers from the development process. As a result, they deliver fewer products to the market, get bogged down in routine, and have little energy left over for ambitious new ideas.
Happily, many QA processes can be automated with third-party services and software. Advanced companies invest in automated products to carve out time for their core activities.
Automation tools not only streamline and accelerate QA procedures but also improve accuracy. Even the most experienced QA specialists are prone to human error, but this is not the case for cutting-edge testing programs. They can effectively detect and correct inconspicuous errors, prevent failure of medical software and devices, test diverse features, scrutinize a wide range of factors, and assemble them all into a comprehensive picture of a product’s performance while providing vastly improved options.
This centralized, all-inclusive control allows developers to achieve the highest possible quality in medical device management software, saving a great deal of time and resources in the process.
Custom Healthcare Solutions
See how we can engineer healthcare software, validate your ideas, and manage project costs for you.

How to Manage Medical Device Software Testing
Several components are fundamental to efficient medical software functioning. The keystone areas of focus in medical software testing include data exchange, system interoperability, and compliance with national and/or international regulations.
You need to make sure that your medical software:
- Features secure communications and transactions, so patient data won’t be easily intercepted or deciphered.
- Is well-protected against security threats and unauthorized access.
- Is well-configured to work smoothly and reliably in combination with other medical systems and hardware, depending on your software system’s purpose and existing configurations.
- Complies with governmental regulations and standards.
Let’s delve into this in more detail.
Guidelines for the Successful Release of Medical Software
Before a medical software solution can be used in a healthcare facility for hospital information management, clinic workflow automation, or driving a medical device, it should be fully approved, verified, and accompanied by the proper documentation.
1. Get Ready to Produce Complete, Well-Elaborated Medical Software Test Documentation
Make sure the testing process is documented so that further action can be taken by developers using the testing outcomes. Your documentation set should include:
- A test plan with specific pass/fail criteria
- Description of verification/validation activities performed on all levels
- Test protocols with specific pass/fail criteria
- A test results report
Once the testing process has been guided and captured with the help of these documents, you can rely on them not only as tangible proof of validation and verification but also as firm ground for further medical software development and improvement of features and qualities.
2. Maintain End-to-End Requirement Traceability in Medical Software QA
Make sure the medical software system is tested under conditions that are very close to real-life clinical settings, environments, and situations.
To accomplish this, you should do the following:
- Interview users and collect user requirements on their use cases and situations.
- Connect business situations, healthcare activities, goals, compliance, and risk management points to specific technical requirements and functionalities.
- Reflect these connections on a test map and build a requirements traceability matrix.
- Ensure that all technical requirements are supported by test cases (scenarios testers go through to identify any issues).
- Prioritize testing activities according to risk level for medical software components.
- Validate software components with the higher risk levels present earlier in the SDLC.
This type of all-around holistic approach allows you to arrange a transparent, manageable testing process and facilitate debugging activities well into the future.
3. Test Medical Data Exchange Security
Different healthcare software systems should operate interchangeably, securely sending medical data and patient records to each other. Safe, predictable transactions ensure consistency in healthcare digital services so zero patient data is ever spoiled, lost, or misinterpreted.
For example, hospital information management systems usually receive and process billing documents generated by third-party software, such as those used by insurance providers. In order to help different systems interact, specific standards of medical data exchange have been established in the U.S.
Safe data transfer that is compliant with existing standards is top priority, and must be subject to quality assurance while preventing data leaks or loss. Remember that any error involving inaccurate interpretation of patient data (PHI) could entail HIPAA violations as well as further costly litigation and/or damage to your business reputation.
The predominant PHI transfer protocols/standards in the healthcare industry are as follows:
- ANSI X12 EDI (EDI in Healthcare): HIPAA-regulated framework for healthcare-related record formatting and carrying out transactions on the organizational level, such as data exchange between hospitals and insurance companies.
- HL7 (Health Level Seven): Another structured messaging unification protocol for bridging and interfacing multiple heterogeneous medical software systems that need to exchange clinical or administrative information, normally within a hospital, clinic, or medical center.
- FHIR (Fast Healthcare Interoperability Resources): Introduced by the HL7 organization, the FHIR app (API method) is now backed by Apple and enables quick integration and interoperability between multiple data systems, including EHRs, mobile apps, medical devices, and more.
- DICOM (Digital Imaging and Communications in Medicine): An international standard regulating all manipulations involving medical imaging information.
Each of these standards has its niche community and ecosystem with a bunch of QA tools, such as official implementation guides, validation software, and more.
What procedures are involved in the quality assurance process for medical data exchange?
- Regulatory: It’s crucial to make sure that implementation guides for any of these standards are followed as precisely as possible. Official documentation is aligned with legal requirements, and once everything is implemented correctly, you can be sure the software will comply with the law at its best. Maintain an audit log to keep track of requirements and verifications.
- Validation and verification: It’s necessary to perform automated testing on all key data processes: message sending, receiving, deciphering, etc. This is to make sure the medical system being tested is correctly and consistently reacting to all transaction and interaction types. Additionally, it’s critical to check all messages generated by medical systems to prove that their blocks are structurally correct and comply with official formatting specifications.
Read also: How to Develop Custom HIPAA-Compliant Healthcare Software
4. Test the Efficiency of Medical-system Interoperability
Organizations with a long track record of healthcare activities usually maintain a mixed bag of modern and legacy medical software systems and devices.
If a new system is going to be added to this kind of zoo, it’s super important to define how all involved pieces and components of the existing medical software/hardware will be mutually integrated with the new system. You need to make sure they’re ready to interact smoothly and free of any errors.
What procedures are involved in testing the interoperability of medical software solutions?
- Define all systems and devices that are going to interact within the facility.
- Create a map of interactions between healthcare software solutions under different conditions: use cases/scenarios, user roles, and more.
- Define the technologies driving different components in various interaction scenarios. For example, some low-level medical devices are programmed in C languages, while databases handling medical records use SQL for inquiries. Web-based apps like patient portals use front-end languages and frameworks…and the list goes on.
- Identify bottlenecks, and test all involved interaction patterns and points to make sure all mixed systems are interfacing well.
Delivered Healthcare Software Portfolio
The leading American healthcare companies benefit from working with us.
Of course, testing these technologies requires the involvement of highly skilled QA engineers and automation specialists. If you’re not looking to establish a long-term QA unit within your organization, consider seeking out an outstaffing partner like TATEEDA.
TATEEDA is a full-cycle healthcare development company capable of organizing and orchestrating the testing process for your medical software in terms of interoperability with other systems. If you need a free consultation, please contact us!
5. Test the System’s Protection from Security Threats
There are myriad security risks to be prevented when implementing a healthcare software solution. Quality assurance pays a great deal of attention to vulnerable areas that can become gateways for malicious invasions and hacker attacks. Here are a few important steps to follow:
- Identify the most vulnerable system components and probable targets for cyber attacks.
- Make sure all necessary protection methods are in place.
- Make sure the software code is well-inspected and doesn’t contain serious security flaws or gaps. Verify that no unauthorized access is possible.
- Check and test the internal network to make sure all layers and entry points are sustainable and hack-proof.
- Evaluate the protection of different components (such as mobile apps) against specific types of threats: jailbreaking, rooting, man-in-the-middle attacks, and others.
It is worth mentioning that a complex software testing process should be designed and conducted by professional QA engineers and executed by experienced medical software testers so that no security gaps are tolerated.
If you need a consultation or help with your current or future software testing, please contact us at TATEEDA. We can provide you with custom quality assurance services for medical devices and/or reinforce your existing project with our qualified software testers who can join your team.
Read also: How to Develop a Custom Medical Staff Management and Scheduling Software System
Methods for Testing Healthcare Software
Since each medical software product is unique, every single one of your projects needs a product-specific testing approach. You need to take into consideration the specifics of manufacturing and implementation, the individual performance parameters of your development team, the demands of investors and clients, and the requirements of regulatory bodies.
Choose from the most popular and effective testing options listed below.
1. Automated Testing
Shifting manual tasks to automation ensures greater accuracy, saves precious time, and simplifies the testing process. This type of testing involves stimulating a software product, observing its reactions, recording results, and drawing conclusions about whether or not the product’s behavior meets all expectations.
2. White-Box Testing
White-box testing focuses upon the internal processes that take place in medical software rather than its external functionality. Increased attention is paid to the handling of overflow, error, and interrupt situations. The automation of white-box testing procedures is necessary due to their complexity and internal, non-obvious nature.
3. Functionality Testing
As opposed to white-box testing, functionality testing is done to make sure all the device’s features work as intended and achieve the planned performance metrics. Special testing environments and scenarios are simulated to observe the software’s behavior under field conditions while verifying and validating its responses.
4. Software & Hardware Validation
After testing the availability and working capacity of all features, the software is put into a real-life or simulated environment to see if it caters to user needs and provides an upscale user experience. The product’s software and hardware are both subject to a thorough examination according to a predetermined set of validation criteria.
5. Verification
The features of the finished product are matched with the requirements set forth at the project launch stage. Measurable metrics are used to gauge the degree of compliance with expected results. Experts involved in the testing process document key steps and findings.

6. Compatibility Testing and the Handling of Errors
Once you know that your device has upscale standalone performance, it becomes necessary to test for compatibility with other devices used in healthcare organizations. It is important to evaluate the product’s performance under critical conditions: for example, internal errors, power outages, and failure on the part of related devices. Your products should have self-regulation and fault-tolerance features as well as the ability to notify users about emerging issues.
Get Help From TATEEDA: Make Sure Your Healthcare Facility Adopts Medical Software of the Best Quality
Of course, quality assurance in healthcare is not a simple thing. It requires a very professional approach that includes a team of professional software engineers.
If you’re looking for quality assurance assistance for your medical software project, you don’t need to hire a full-time in-house team of software developers and testers. You can easily borrow them from a medical software testing company like TATEEDA.
TATEEDA is a U.S.-based company that offers a variety of IT services to healthcare providers and companies, including:
- Full-cycle custom medical software solutions development (web, mobile, desktop, IoMT, cloud.)
- Project reinforcement services, including QA outstaffing and staff augmentation.
- Turnkey medical software testing services (desktop, mobile apps, and more).
TATEEDA can help you develop and test different types of medical software solutions, including:
- Nurse Appointment Management Solutions
- Electronic Health Records (EHR)
- Hospital Information Systems (HIS)
- Patient Portals
- Laboratory Information Management Systems (LIMS).
- Pharmacy Management Systems
- Telehealth and Remote Health Monitoring Apps
- IoMT Solutions
Can You Hire TATEEDA for Full-cycle Healthcare Software Development Services, Including QA?
Sure! This would be the best option, as TATEEDA offers a diversified team that brings you a turnkey experience while delivering complex medical solutions from scratch. Fully engaged in your project from the very beginning, TATEEDA ensures the most organic possible integration of QA specialists into your project’s flow, thus providing you with the best quality assurance results.
If you’re interested in a medical software QA project of any type, talk to us. Let us assist you with the testing process for software for medical devices!











