How to Implement an AI-first Strategy in US Healthcare Companies

If you’re trying to make AI genuinely useful in healthcare staffing, this article gives you a clear way to think about it without getting lost in tools, buzzwords, or “pilot theater.”
You’ll walk away with a practical mental model for where AI actually earns its place in HR workflows, how to roll it out without breaking trust or compliance expectations, and what to measure so you can prove it’s improving day-to-day operations rather than creating new work.
An AI-first healthcare strategy is not “everyone, please open ChatGPT,” while your real hiring data and processes are scattered across five places at once. That approach creates daunting motion and hassle, not momentum. It can look busy but not productive; it rarely makes a meaningful change to time-to-fill, nurse utilization, or the number of stalled onboarding packets.
As experts in custom healthcare HR software development, we offer a unique perspective on how AI is used in medical facilities and health companies to automate and refine staffing processes.
In many US healthcare organizations, staffing and HR data get split across a mix of systems, for example:
- An ATS like iCIMS or Greenhouse for applicants
- An HRIS like Workday or UKG for employee records
- A scheduling layer (often UKG again, or a comparable workforce tool) for shift coverage
- Shared storage like SharePoint or Google Drive for documents and templates
- “The audit trail” living in email threads, approvals, and forwarded attachments.
Then there’s the semi-analog “last mile” that still shows up everywhere:
- Scanned licenses and certification PDFs
- Faxed forms and printed checklists
- I-9 and onboarding packets that start on paper
- Handwritten notes that never become structured fields.
AI can’t reliably speed up a workflow that isn’t connected or standardized. If you want fewer stalls and measurable throughput improvements, you typically start by turning the workflow into something AI can assist end-to-end. That’s where AI software development services come in: unifying data sources, enforcing rules, and keeping an audit-friendly record of what happened and why.
So, what is an AI-first strategy? In healthcare software development companies, it is an operating shift where AI becomes part of how work runs day-to-day. Not as a toy, not as a slide deck. As infrastructure that shapes:
- How tasks move through a workflow
- How decisions are proposed and verified
- How systems share data under strict rules and logging.
Put two equally capable healthcare HR teams side by side. The team with well-governed healthcare AI HR copilots and tightly bound agents will usually move faster. More outreach completed → Fewer no-shows → Cleaner screening notes → Better matching.
The other team can still win…if it has unlimited recruiter capacity. Almost nobody does!
Table of Contents
The Common Failure Pattern: Pilots Everywhere → Impact Nowhere?
A lot of organizations try “a little AI” across ten places. A chatbot here. A summarizer there. A scoring widget bolted onto an ATS. The result is fragmented value and growing risk.
In healthcare, most healthcare AI failures, or the downsides of a flawed strategy, show up early because the constraints are real: HIPAA, multi-system identity, credentialing rules, license verification, background checks, and hard operational deadlines.
This is why a healthcare AI-first strategy should mean one thing:
- Measurable outcomes: Track a small set of operational metrics that matter in healthcare HR, for example, time-to-fill, drop-off rate, interview no-shows, and credentialing cycle time, then tie every AI change back to those numbers.
- Fewer experiments: Stop scattering small pilots across ten teams; pick a short list of workflows that actually hurt when they stall (staffing, credentialing, scheduling), then focus effort there.
- More repeatable workflows: Build one “same steps every time” process that can run across facilities, roles, and seasons, instead of one-off automations that break the moment inputs change.
- Clear ownership: Assign a single accountable owner per workflow (not “the AI team”), so decisions, data quality, and adoption have a real name attached.
- Guardrails: Define what AI can do, what requires human approval, what data is allowed, and what must be redacted or blocked; document it so the process stays consistent under pressure.
Why Deploying a Public-facing AI Can Be the Wrong Starting Point for a Healthcare Company
Healthcare leaders often feel pressure to start where AI is visible: patient chat, automated service, intake bots, flashy assistants. The problem is the blast radius. A small mistake can become a compliance incident or a trust event, leading to reputational and financial loss.
Here are typical failure modes when you start externally instead of internally:
| Failure mode | What it looks like | Likely outcome |
|---|---|---|
| Confidently wrong answer | AI “explains” eligibility, coverage, or policy without valid evidence | Complaints, escalations, regulator attention |
| Biased recommendation | AI systematically favors certain profiles or filters out others | Fairness concerns, audits, rollback |
| Data-handling slip | Sensitive information shows up in prompts, logs, or the wrong screen | Security incident, breach response, legal exposure |
Internal workflows give you a safer proving ground. Inputs are more standard. You can add approval gates. You can train teams to treat output as a draft plus evidence, not a verdict. Most importantly, you can measure value quickly without putting patients or brand trust on the line.

Learn more: ➡️ Best AI Development Companies for the US Market
A Phased Roadmap from Pilots to an AI-first Business in Healthcare
If you want an AI-first business in healthcare, think in phases. Not because phases are fashionable, but because healthcare workflows have dependencies. Data has to be accessible. Policies must be explicit. Someone must own the outcome…
“The best AI in healthcare staffing is boring in a good way. It produces the same outputs for the same inputs, it never ‘forgets’ a document, and it doesn’t skip steps. The human owner’s job is to define the path for edge cases: missing license, conflicting dates, expired cert, or an exception request. The AI’s job is to route, not to guess.”
— Slava K., CEO at TATEEDA
Phase 1: Alignment, pick workflows that hurt when they stall
Choose 2–3 workflows with a real “cost of delay.” Healthcare HR and staffing has plenty: candidate rediscovery, screening, interview scheduling, credential packet collection, and onboarding coordination. Assign one accountable owner per workflow. Then define rules early: which data is allowed, what must be redacted, what actions require a human sign-off, and what gets logged by default.
This is also where you decide what AI is allowed to do. Draft outreach messages? Fine. Auto-approve a credential exception? Probably not. If the rules are fuzzy, the system will be fuzzy…
Phase 2: Foundations, connect the systems of record
In healthcare HR, “systems of record” usually mean an ATS, an HRIS, scheduling, credentialing, and document storage. Sometimes it also includes a CRM and internal workforce planning spreadsheets that everyone swears are temporary.
Your foundation work is unglamorous but decisive: identity mapping, role taxonomy cleanup, consistent credential naming, and controlled data access. Add observability early. You should be able to answer, in plain language: what data was entered, what AI was produced, who approved, what system was changed, and when.
Phase 3: Controlled Automation, Move from Copilot to Bounded Agents
Copilots help humans write and summarize. AI multi-agents help workflows finish steps. That distinction matters in staffing because the bottleneck is not “lack of text,” it is lack of completed work: unanswered outreach, incomplete profiles, missing documents, unbooked interviews.
This is where medical AI-first starts to look real. A controlled agent can do a narrow set of tasks, inside strict rules, with escalation paths. For example: “Collect missing documents, check completeness, route exceptions to a recruiter, and write back status updates.”
Two grounded examples from the staffing context:
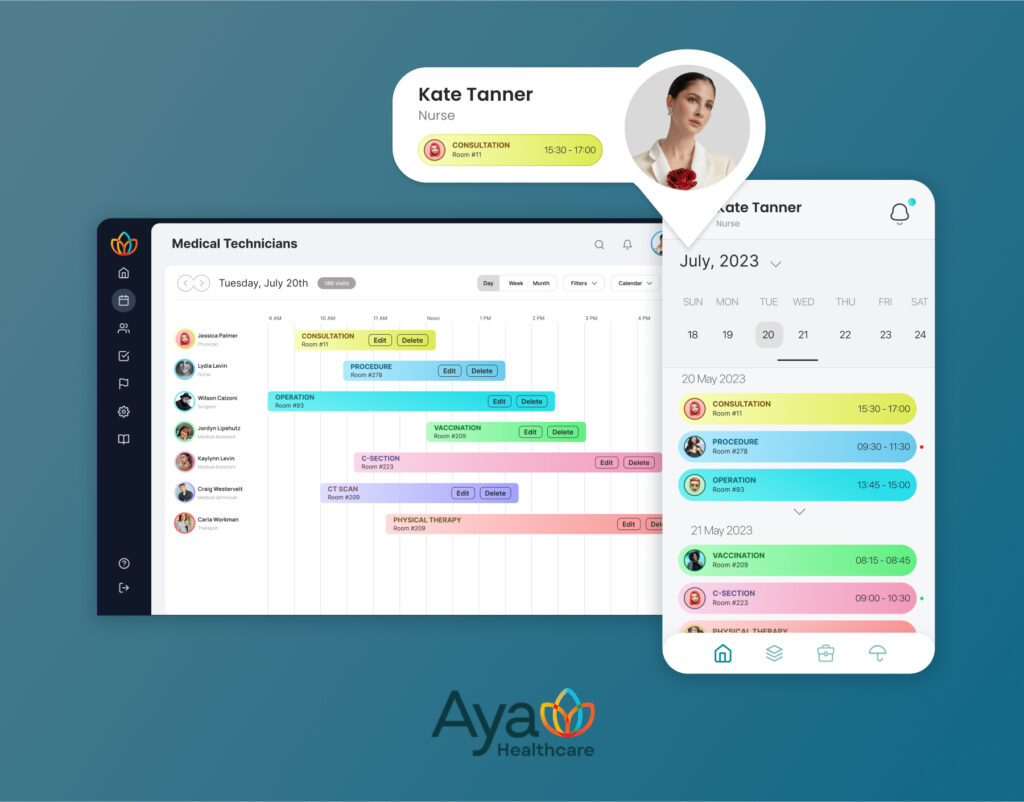
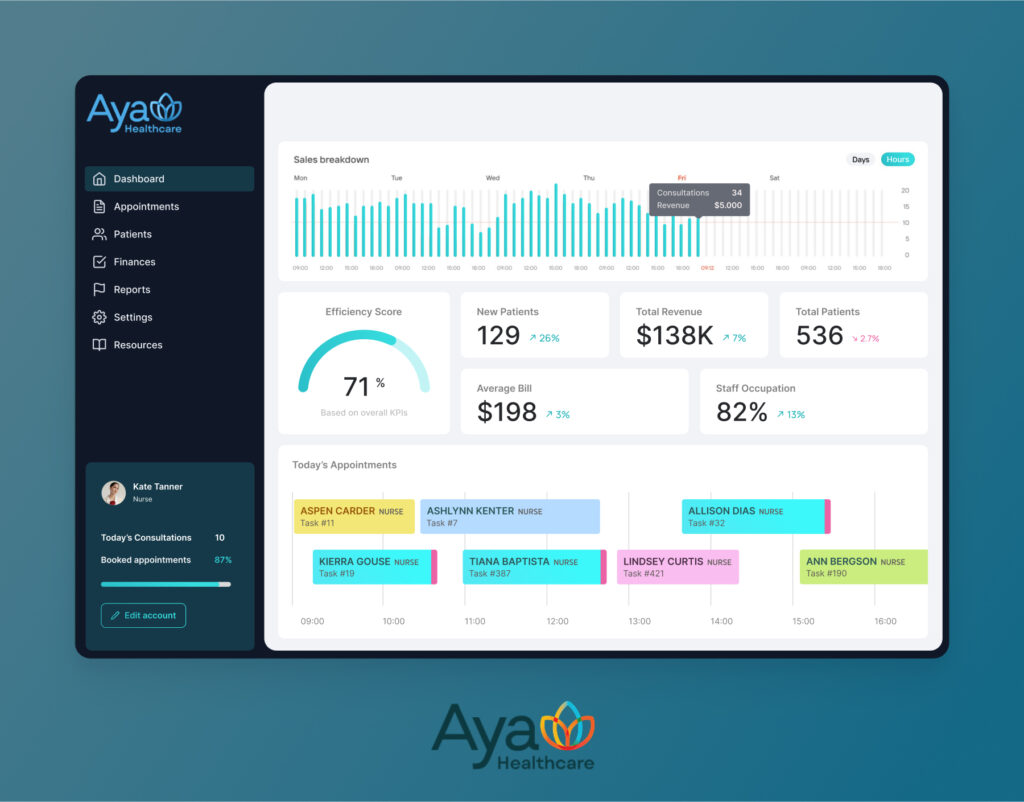
Example 1: AYA Healthcare staffing workflows (travel nursing match logic)
In travel nurse staffing, matching is a constrained problem: specialty, license state(s), start date, shift type, facility rules, compliance items, and availability. AI can help surface better matches faster, but only if the scoring rubric is explicit and the workflow is auditable. In our work with AYA Healthcare, AI-style components can be used to assist matching and qualification scoring while keeping human review for edge cases and exceptions.
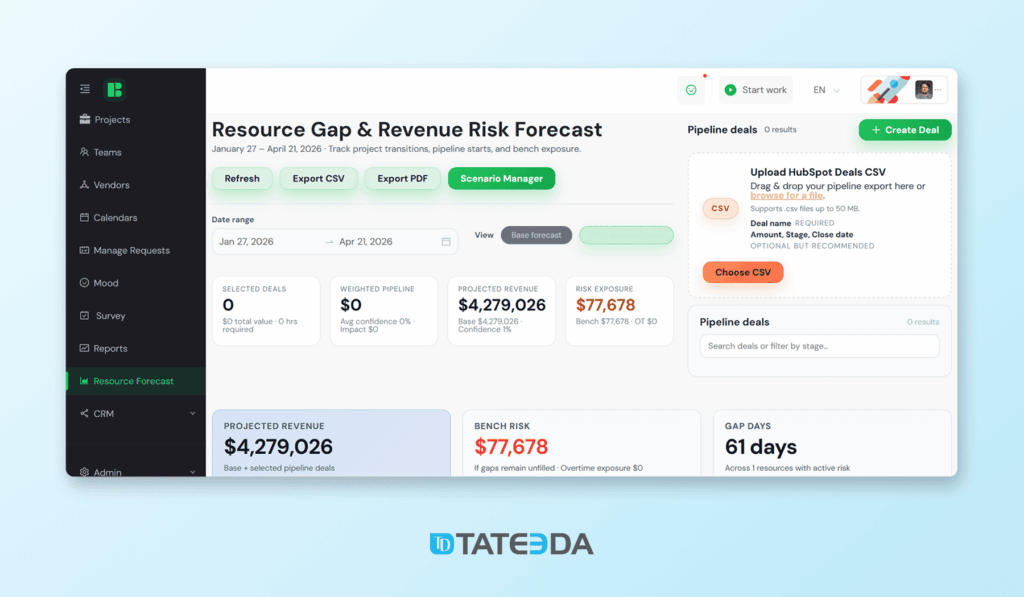
Example 2: BeOnBoard (BoB) internal operations and skill scoring
BoB is a web-based small business suite that blends CRM and operational tracking. AI can add practical lift here too: skill scoring, intake structuring, faster sorting of leads or candidates, and consistent summaries. The key is that the AI output is treated as assistive signals and structured drafts, not a final authority.

Phase 4: Selective externalization, only after internal controls work
Once internal controls are stable, you can externalize carefully. Patient-facing AI, candidate-facing voice intake, or automated service becomes safer when you already have the internal playbook: audit logs, escalation rules, human review pathways, and monitoring that catches drift and abnormal behavior.
The Biggest Blockers are Execution Bottlenecks, not Model Quality
Most initiatives stall because the organization cannot run AI as a managed capability. Not because “the model is dumb.” In healthcare, the repeat offenders are predictable:
- Ownership gaps: no one owns the workflow outcome end-to-end
- Data disorder: duplicate profiles, inconsistent credential fields, and missing timestamps
- Governance thinness: unclear rules about PHI, retention, access, and logging
- Change friction: teams do not trust the output, so it becomes extra work.
This is why a healthcare AI-first strategy starts with workflow discipline, not prompt tricks.

Learn more: ➡️ Top 20 Healthcare Technology Trends in 2026
Where AI Agents belong First in Healthcare, HR, and Staffing
Start with workflows that are repetitive, bounded by policy, and easy to audit. Healthcare staffing offers several. One useful mental model: AI handles the “clerical momentum,” humans handle judgment and exceptions.
Good early fits:
- Candidate rediscovery and shortlist building with explicit constraints
- Screening intake (chat or voice) using structured questions and clear disqualifiers
- Interview scheduling coordination plus reminders
- Credential packet collection, completeness checks, and status updates
- Onboarding document routing with acknowledgements and training assignments.
Notice what is missing: autonomous final decisions on employment eligibility, compliance exceptions, or anything that could create legal exposure without a human sign-off.
What “Good” Looks Like: Performance, Compliance, and ROI
Healthcare leaders care about repeatability and traceability because that is what holds up under review. So measure like a production system, not a demo.
- Operational impact: cycle time reduction across screening, scheduling, and onboarding; fewer no-shows; fewer stalled packets; lower rework.
- Audit readiness: log completeness (inputs, outputs, approvals, actions); clear data lineage; evidence attached to decisions where needed.
- Business value: reduced overtime pressure from open shifts; higher recruiter throughput; avoided backlogs; fewer compliance escalations caused by missing documents.
If those measures do not move, you do not have an AI-first approach. You have scattered tools and uncertain risk.

What to Do Next: AI-first Software Development with TATEEDA
If you want to move toward AI-first healthcare without creating new compliance headaches, start internal-first. Pick one workflow. Lockdown rules. Measure impact. Then expand.
A practical checklist before you scale:
- What workflow are we accelerating, and what does success mean in numbers?
- Which data sources are allowed, and who owns quality and access?
- Where are verification gates, and what gets escalated to a human?
- What record would satisfy an auditor if asked how a decision was made?
How TATEEDA helps
TATEEDA supports US healthcare organizations that want AI to land inside real operations. That includes designing AI-assisted staffing workflows, building bounded AI agents for HR, integrating with ATS and HR systems, and implementing HIPAA-aware controls such as redaction, least-privilege access, and audit-friendly logging. The goal is simple: move from “interesting pilots” to a system your teams can actually run and trust.
To make that happen, we bring the full delivery capacity for AI-assisted software development needed to take an AI idea from concept to production, including:
- AI architects and engineers to design agent workflows, scoring logic, data boundaries, and evaluation approaches
- Full-stack development for web applications and internal portals used by recruiters, staffing coordinators, and admins
- UI/UX design for HR-facing dashboards, intake forms, and workflow screens that teams can adopt quickly
- Integration software engineering across ATS/HRIS, scheduling, credentialing, document storage, and communications tools
- Cloud delivery on AWS, Azure, or Google Cloud with secure environments and deployment automation
- Nearshore software development services with senior teams in Eastern Europe and LATAM for consistent delivery across time zones
- QA and testing (including workflow, regression, and security-focused checks) to keep releases stable in high-stakes environments.











